This month, SAMHSA announced $200 million is now available nationwide for the Certified Community Behavioral Health Clinic (CCBHC) Expansion Grants. Not only is this a $50 million increase from 2019 funding, but it also advances the program to be available in all states. While clinics from all 50 states may apply for grants, SAMHSA indicates they will prioritize the 24 states that received CCBHC planning grants in 2016. To see if your state is included in the 24 receiving priority, please reference who is eligible for expansion grants from The National Council. The CCBHC model intends to provide more access to mental health and addiction services to vulnerable populations. With this increase in funding, more behavioral health care will become available to individuals nationwide. So, let’s back up: what is a CCBHC?
The CCBHC Model Defined
Certified Community Behavioral Health Clinics provide a range of behavioral health services. They have a designated provider type in Medicaid, allowing them to receive enhanced reimbursements. The model began under the Protecting Access to Medicare Act of 2014, which established a 2-year, eight-state initiative based on the Excellence in Mental Health and Addiction Act1. The Excellence Act is centered on providing access to mental health and addiction services through CCBHCs while improving Medicaid reimbursement. Improved reimbursement rates allow more people in need to access necessary care. As an underserved population, Medicaid recipients struggling with complex mental health and substance use disorders often can’t access quality care. CCBHCs work not only to fill this gap but also to provide a comprehensive and integrated model for care. The hope behind the model is to provide stability, access, and necessary treatment for these vulnerable behavioral health patients.
As described by The National Council2, CCBHCs must provide the following nine comprehensive care requirements:
- 24/7/365 crisis mental health services
- Screening and risk assessment
- Patient-centered treatment planning
- Outpatient mental health and substance use services
- Primary care screening and monitoring of key health indicators/health risk
- Targeted case management
- Psychiatric rehabilitation services
- Peer and family support
- Tailored care for active-duty military and veterans
SAMHSA3 states they expect “this program will provide comprehensive 24/7 access to community-based mental and substance use disorder services; treatment of co-occurring disorders; and physical healthcare in one single location.”
Who Receives Care at a CCBHC?
Any individual in need of behavioral health services can receive care at a CCBHC. This includes, but is not limited to, individuals with mild to serious mental illness, long-term chronic addiction, and substance use disorders. The enhanced Medicaid payment method allows organizations to receive reimbursements more effectively. Prior to this model, it was difficult for Medicaid-recipients to receive quality behavioral health coverage. Therefore, Medicaid-recipients largely benefit from care at CCBHCs. Additionally, CCBHCs provide care to individuals, regardless of their ability to pay. CCBHCs provide service to those who are insured, uninsured, and on Medicaid.
How to Become a CCBHC:
SAMHSA describes 6 program requirements for CCBHCs. The 2020 Funding Opportunity Announcement defines the following requirements:
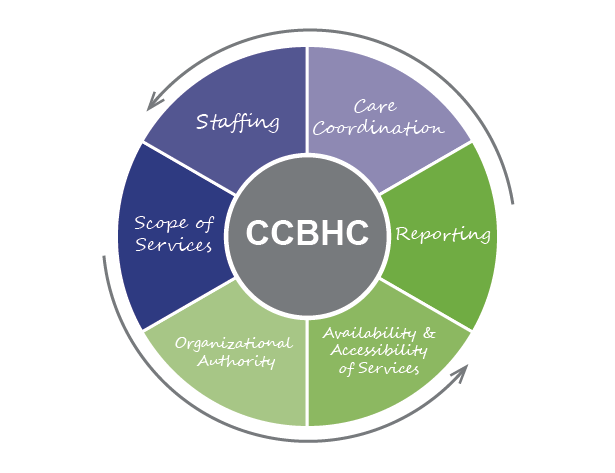
- Staffing
- Availability and accessibility of services
- Care coordination
- Scope of services
- Quality and other reporting
- Organization authority, governance, and accreditation
If your organization meets these requirements, visit the SAMHSA website to apply for the Certified Community Behavioral Health Clinic Expansion Grant.
Resources to Help CCBHCs
If your organization follows an integrated, comprehensive care model such as a Certified Community Behavioral Health Clinic, your resources need to support the care you provide. For example, CCBHCs have specific procedure codes for billing. SAMHSA also requires particular reporting for CCBHCs, including certain data selection and performance measurements. Electronic Health Records play a critical role in these billing and reporting requirements. Patagonia Health not only supports but easily automates the unique reporting and billing that’s required when an organization becomes a CCBHC. To find out more about how our solution can support your organizational needs, contact us today.



